🩺 The Pulse: Scaling AI in Real Clinical Workflows – Physiotherapy, Cardiology
Plus: Building a smarter documentation template with Heidi AI
1. Triage – Your Fortnightly Rundown
Hey Pulse Readers, we’re back! And we will be in your inbox every second Wednesday from now on. Let’s dive right into it:
promising results in AI physiotherapy clinic with expansion across the UK,
what 11 randomised trials found about the impact of AI in cardiology clinical outcomes and operations,
and how you can get Heidi to write notes that are more “like you”.
2. Case Study – Your Fortnightly Practical
Image Source: Heidi Health
Designing Documentation That Matches Complex Consults
Case Presentation: Harry is a busy GP in Aotearoa who recently started offering adult ADHD assessments after the 1 February 2026 rule change by the New Zealand Government.
These appointments are long, often over 60 minutes and across multiple visits. He found that his standard GP note templates (SOAP style, short problem lists) do not fit the structure of an ADHD assessment or the f/u plan.
He is stuck rewriting the same sections every time and has to stay behind after hours to finish his notes.
Approach: Build a fit-for-purpose ADHD assessment template by uploading a de-identified example document to Heidi, then iterating until the output matches how you want to document.
1. Pick a “gold standard” example note
Choose one ADHD assessment note you are happy with (3rd party or self-drafted), focusing on headings and structure (not patient specifics). Aim for the exact output style you want to reuse as your baseline structure.
2. De-identify properly, do not be sloppy
Replace names, NHI, DOB, address, and other unique identifiers with placeholders (for example, [PATIENT], [DOB], [ADDRESS], [DATE]).
3. Upload and create a template in Heidi
Use Heidi’s template creation workflow to upload your de-identified note and have Heidi generate a “Adult ADHD assessment” template according to your preferred structure and wording. Heidi supports building templates through conversation and adapting from uploaded existing templates. Alternatively, reach out to the Hendrix team, and they can do this for you.
4. Test and refine
Run a dummy case through the template, check the output, then adjust the template instructions until it reliably produces the level of detail you need and you have to make as little edits as possible before copying and pasting into your PMS or EHR. You will still need to review the notes for accuracy in any case.
Save and favourite it for fast access.
Outcomes: With a dedicated ADHD template built from his own documentation style, Harry stops re-writing the assessment from scratch each time. His consult notes become consistent across clinicians, easier to review at follow-up, and super quick to complete, which matters when assessments routinely take > one hour.
Instead of fighting his usual GP templates, he now has a repeatable workflow that fits the new reality of ADHD care in primary care.
Disclaimer: Hendrix Health is the official New Zealand partner for Heidi Health.
3. The Pulse - Your Fortnightly Update
AI Physiotherapy Clinic Now Expanding Across 11 NHS Regions After Pilot Programmes
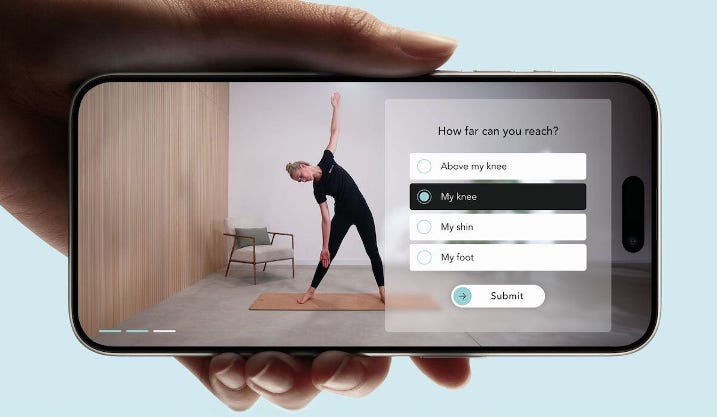
Flok Health, an AI powered physiotherapy clinic, has expanded across 11 NHS regions to provide patients with same-day video appointments for back pain via a smartphone app. This follows large-scale pilots in Scotland and England in early 2025, and the rollout now covers more than 2.4 million patients across England.
Image Source: Flok Health
The service begins with a mobile phone video assessment, with the AI system evaluating patient symptoms. If approved, they receive weekly video appointments with the AI physiotherapist, available at any time. Patients can also send voice messages to the clinical team and receive responses during working hours.
Those with more complex symptoms have a further telehealth assessment with a clinician before digital treatment; or otherwise, referral to a more appropriate NHS service. This keeps clinician time focused on higher complexity care.
Key Features:
Waiting list impact: In one of the pilots, waiting lists for back pain were cut by more than half, and waits for all MSK conditions fell by 44 percent in under 10 weeks.
End-to-end pathway: The AI physiotherapist manages patients from initial assessment through treatment and discharge, recording interactions and outcomes into the patient’s EHR.
Regulatory readiness: Class IIa medical device approval under EU regulations supports autonomous delivery of diagnostic decisions and treatment pathways without requiring clinician input.
Patient reported improvement: Average MSK-HQ score improvement of 6.16 points, with anything above 5 considered to be clinically significant.
Implications for the Health System and Clinicians:
For the UK, this is a clear signal that commissioners will back regulated, integrated digital pathways where the operational case is strong. For ANZ services watching from a distance, the useful lesson is the combination of regulatory clearance, and measurable waiting list impact.
In the long term, the real test will be sustaining outcomes across diverse populations, maintaining clinical oversight, and ensuring equitable access for patients who might not engage well with smartphone-delivered care.
AI in Cardiovascular Care: What 11 Randomised Trials Tell Us
A new systematic review in Journal of the American College of Cardiology examined randomised controlled trials of the application of AI in cardiovascular care. It aims to investigate AI’s impact on cardiology patient outcomes and health systems.
Image Source: Journal of the American College of Cardiology (JACC)
Key Findings:
ECG: > 50% of the trials focused on ECG-based AI, mainly to screen and flag higher-risk patients earlier, prompting early detection or escalation. One trial showed reduced 90-day mortality, but another trial showed worse outcomes. Overall, modest clinical benefits and often seen in high-risk subgroups.
Computed Tomography: CT-based AI tools were used to support coronary risk assessment and procedural planning. It helped reduce unnecessary downstream invasive testing, and promoted consistent preventive care (e.g. statin use) when actionable findings are identified.
Echocardiography: Results were mixed. For routine echo workflows (e.g. EF assessment), AI performed as well as sonographers and helped save time, but performance was not strong enough in specialised context such as stress echo for coronary disease detection.
Evidence and reporting gaps: Only 11 out of 930 RCTs (2021 to 2024), met inclusion criteria. None of which reported patient-reported outcomes (e.g. quality of life, symptoms) and only 5 RCTs declared adherence to AI-specific reporting standards (CONSORT AI or SPIRIT AI). Many studies had moderate to high risk of bias linked to industry funding or financial interests.
Implications for Healthcare Systems:
AI in cardiology shows promise for screening, early detection, standardised interpretation, as well as operational / workflow efficiency. More high-quality evidence is needed to validate AI’s effectiveness in hard clinical outcomes (e.g. treatment response rates, patient-reported outcomes) before widespread clinical reliance and scaling.
Read the full review here.
4. Vitals – Quick Bytes
AI in ED sepsis, early alerts and smarter diagnostics, but limited evidence
A narrative review outlines how AI could support sepsis care in the emergency department, from early warning alerts (e.g. TREWS) to improving diagnostic work ups such as targeting blood cultures and combining biomarkers with routine data (for example Sepsis ImmunoScore). The main caution is that most sepsis AI has only been validated in observational studies, with limited randomised evidence. The incomplete ED data capture and generalisability also remain challenges. The takeaway is simple: promising tools, but they still need rigorous trials and careful workflow integration before wide rollout.
US-based Optain Health acquires EyePACS to scale AI retinal screening in primary care
Optain Health is combining their AI-powered robotic retinal imaging with EyePACS’ teleophthalmology network, expanding retinal screening in primary care and community clinics. A portable, robotic camera captures retinal images at the point of care to detect diabetic retinopathy, glaucoma, and age-related macular degeneration. Optain is also positioning this platform for “oculomics”, using signal from the eye to inform broader cardiometabolic risk assessment. The combined platform’s specialist multi-condition grading, EHR integration and analytics helps support population health programmes. (fiercehealth.com)
We’d love to hear your thoughts, so join the conversation by leaving a comment below:
Stay tuned for more insights in next week's edition of The Pulse.
Have a great day & see you in two weeks!
Your Hendrix Health Team